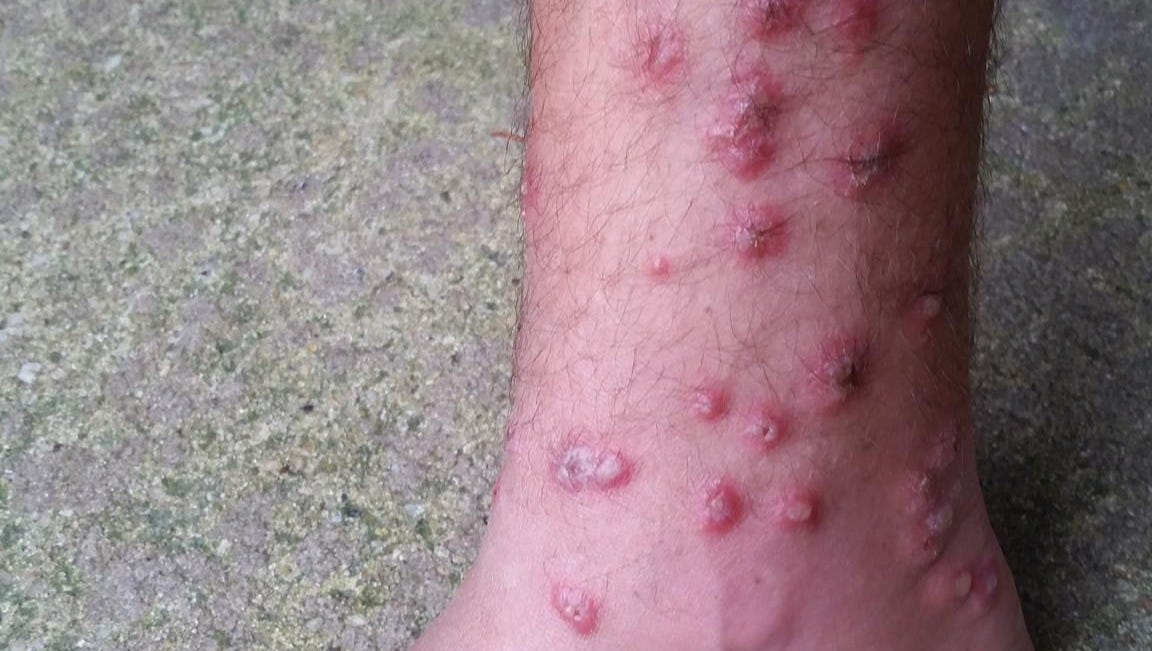
This confirmed the diagnosis of swimmer’s itch. She also saw a dermatologist who performed a skin biopsy that revealed the presence of cercariae within the skin. She went to her primary care doctor who recommended use of oral antihistamines and moisturizing lotion. Her skin felt hot and she noticed the symptoms were worse in the morning. The next day, she developed an itchy rash on her face and shoulders. Apply waterproof sunscreen as this may protect the skin from larvae that cause swimmer’s itch.Ī 41-year-old woman went swimming in a lake where there was a lot of vegetation present near the water surface.Towel dry and shower immediately after leaving the water. 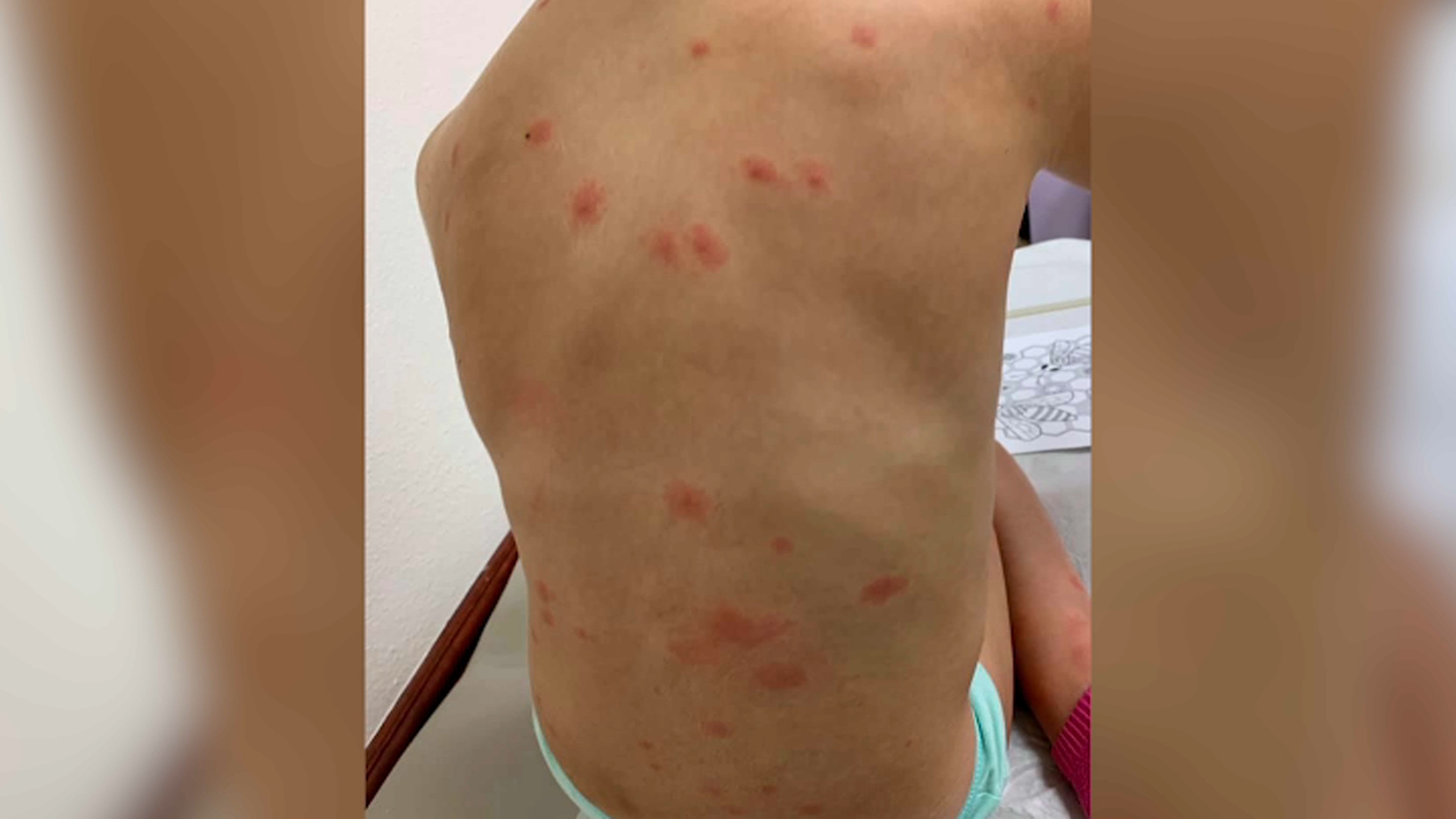
Prolonged time in water is a risk factor for swimmer’s itch and may result in more severe symptoms.Avoid swimming in areas where posted signs warn that swimmer’s itch is a problem.Avoid swimming in marshy or shallow waters whenever possible, as there are more snails in these areas.Do not feed birds in areas where people swim.Both options are free for the public, and available 24 hours a day. If symptoms do not resolve or if the rash appears to be getting infected, seek medical attention.įor questions about swimmer's itch, go to or call 1-80. Most cases of swimmer’s itch will resolve within 1 to 2 weeks with simple home treatment. Avoid excessive scratching of the itchy areas because this can lead to a skin infection. More severe cases may require treatment with prescription medications. Topical steroids such as hydrocortisone cream and antihistamines such as diphenhydramine (Benadryl®) can be used to treat itching. Baking soda baths and pastes can be helpful as well. Cool compresses and soaking in Epsom salts or oatmeal baths can soothe the rash. Drying your skin with a towel, instead of air drying, may help remove the larvae from the skin. If you suspect swimmer’s itch, you should take a shower if you have not already done so after getting out of the water. Most cases of swimmer’s itch can be easily treated at home. Severe symptoms, including fevers, diarrhea, and nausea, are rarely reported to occur in patients with swimmer’s itch. Because it is an allergic reaction, swimmer’s itch is not contagious. While the rash is uncomfortable, it is generally self-limited and not dangerous. This helps to differentiate swimmer’s itch from seabather’s eruption, which primarily affects the skin under the swimsuit. The rash typically involves areas of the body that are exposed to the water, with areas of skin covered by bathing suits being spared. The rash may appear similar to pimples, chickenpox, or blisters, and is often red and itchy or burning in nature. Within a few minutes to a couple of days after swimming in contaminated water, a rash can develop. The larvae die, but their presence in human skin can cause the characteristic itchy rash. The larvae are able to painlessly burrow into human skin, but the parasites are not able to survive there. The larvae can be encountered by swimmers, particularly in shallow and marshy areas, although the tiny larvae are too small to see. If the parasite eggs are released into or near the water, they can hatch into larvae, which can then infect snails. The adult parasites produce eggs, which are passed into the water from the feces of these animals. Several species of birds (geese, ducks, gulls) and mammals (beavers) that live near water can be infected with parasites in their blood. Swimmer’s itch is a water-borne parasitic disease, and the normal life cycle of the disease-causing parasite involves different animals. This is called swimmer’s itch or cercarial dermatitis. When swimmers come into contact with these parasite larvae, the larvae can burrow under the skin, causing an allergic reaction that manifests as itching and rash. Infected snails can then release the larvae back into the water. Snails found in freshwater, and rarely in salt water, can be infected by juvenile parasites (cercarial larvae) that are present in the water.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
